Traumatic Brain Injuries and Their Relationship to Suicide in Veterans
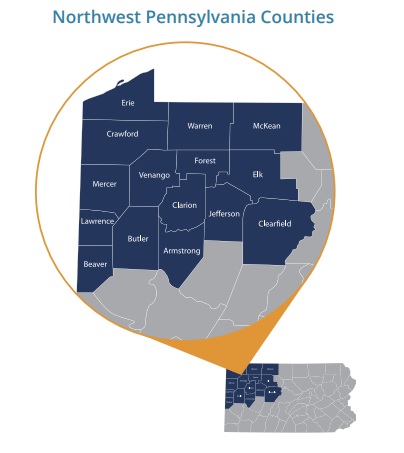
The Northwest Pennsylvania (NW PA) Veteran Suicide Prevention Program operates on a three-pronged approach involving healthcare providers, community organizations, and Veterans and their families in the 15 counties of NW PA.
This article summarizes a research presentation by Lee Wagner, Senior Program Implementation Specialist, and explores the following topics:
- What defines a traumatic brain injury (TBI)?
- The occurrence of TBIs in military personnel within the last twenty years
- The connection between TBI and suicidal ideation (SI)
- Best practices regarding TBI and SI in Veterans
Read time: 7 minutes
A pdf of the presentation, including sources, is available for download.
What is a TBI?
 A TBI can result from a bump, blow, jolt to the head, or a penetrating head injury. The primary symptom of a TBI is cognitive impairment; however, physical and sensory symptoms can emerge in even mild cases of TBI and may become progressively worse in moderate to severe cases.
A TBI can result from a bump, blow, jolt to the head, or a penetrating head injury. The primary symptom of a TBI is cognitive impairment; however, physical and sensory symptoms can emerge in even mild cases of TBI and may become progressively worse in moderate to severe cases.
Clinical signs of altered brain function can include:
- A period of loss or decreased consciousness
- Any loss of memory for events immediately before or after the injury
- Neurological deficits such as muscle weakness, loss of balance and coordination, disruption of vision, change in speech and language, or sensory loss
- Any alteration in mental state at the time of the injury such as confusion, disorientation, slowed thinking, or difficulty with concentration
Source: https://www.cohenveteransbioscience.org/traumatic-brain-injury/
Instances of Reported TBIs in Military Personnel 2000-2019
From 2000-to 2019, 413,858 United States military personnel worldwide experienced a TBI; 82.8% were considered mild, 9.8% moderate, and 2.3% penetrating or severe (Shura et al., 2019). It’s worth noting that of those who experienced a TBI
- Approximately 80% were first-time TBI cases occurring in non-deployed settings such as training activities.
- Sustaining a TBI from an explosive blast was a common incident within the military community.
- Of the 770,000 Veterans of Operations Enduring Freedom and Iraqi Freedom (2001 – 2014) who sought care from a VA Medical Center, nearly 60,000 were evaluated or treated for TBI-related conditions.
The Relationship Between Traumatic Brain Injury History and Recent Suicidal Ideation in Iraq/Afghanistan-Era Veterans
 Published in 2019 in Psychological Services, this research article investigated the relationship between TBI and recent SI after adjusting for demographics, sleep quality, PTSD, and depression. Areas for investigation included:
Published in 2019 in Psychological Services, this research article investigated the relationship between TBI and recent SI after adjusting for demographics, sleep quality, PTSD, and depression. Areas for investigation included:
- The effects of TBI on recent SI on Veterans serving between 2001 and 2014
- Comparing lifetime TBIs and deployment related TBIs, and the impact of both scenarios
- Compared those who sustained multiple lifetime TBIs with those who reported no TBI or a single lifetime TBI
- Screening for factors beyond deployment related TBI occurrences (demographics, depression, PTSD, and sleep quality).
Findings for TBI and SI in Veterans included the following:
- A lifetime history of TBI was not found to be a significant predictor for recent SI after adjusting for depression, demographics, sleep quality, and PTSD.
- A history of multiple TBIs was associated with recent SI compared to those with no history of TBI.
- While sustaining a TBI may not directly impact SI, ailments that stem from a TBI and lifelong stressors do.
- TBI can lead to poor sleep habits
- TBI can be a contributing factor to major depressive disorder (MDD)
- Both poor sleep and MDD are risk factors for SI
Treatment and Next Steps
 Most TBI survivors (75%) experienced a mild brain injury that involves a brief change in mental status or consciousness but with no structural damage to the brain. Mild TBI symptoms may be subtle, ranging from no apparent deficit to temporary personality changes; however, individuals may experience lifelong cognitive or psychological challenges. Frontline screeners should be aware of the following:
Most TBI survivors (75%) experienced a mild brain injury that involves a brief change in mental status or consciousness but with no structural damage to the brain. Mild TBI symptoms may be subtle, ranging from no apparent deficit to temporary personality changes; however, individuals may experience lifelong cognitive or psychological challenges. Frontline screeners should be aware of the following:
- Addressing MDD and poor sleep habits in those veterans with a TBI can help reduce SI risk factors.
- Screening for lifetime TBI and deployment related TBI can help the provider determine medical and behavioral health treatment options.
Share Our Vision and Get Involved
Our Vision: The work of the Northwest Pennsylvania Veteran Suicide Prevention Program will result in resident Veteran suicides being reduced to zero by the end of the project period (August 31, 2025).
Whether you identify as a healthcare provider, community organization, or Veteran, there are several opportunities through the NW PA Veteran Suicide Prevention Program and PERU to connect to resources, participate in educational training, and promote harm reduction strategies. We are actively recruiting healthcare and community partners to work with us in meeting our goals and objectives. To learn more, visit the program website at theresilientveteran.org.
Need Help? Know Someone Who Does? Contact the National Suicide Prevention Lifeline at 988 or use the online Lifeline Crisis Chat. Both are free and confidential. You’ll be connected to a skilled, trained counselor in your area.

