Considerations of Universal Suicide Risk Screening in Primary Care Settings
 The Northwest Pennsylvania (NW PA) Veteran Suicide Prevention Program operates on a three-pronged approach involving healthcare providers, community organizations, and Veterans and their families. In this article, which summarizes a recent presentation by PERU program implementation specialist Alisa Balestra, Ph.D., the following topics are explored:
The Northwest Pennsylvania (NW PA) Veteran Suicide Prevention Program operates on a three-pronged approach involving healthcare providers, community organizations, and Veterans and their families. In this article, which summarizes a recent presentation by PERU program implementation specialist Alisa Balestra, Ph.D., the following topics are explored:
- Why suicide risk screening in primary care settings saves lives,
- Barriers to suicide risk screening and strategies for successful implementation, and
- Special considerations for suicide risk in rural areas.
Read time: 5 minutes
A pdf of the presentation, including sources, is available for download.
Why is universal suicide risk screening important?
 In 2007, The Joint Commission (TJC) released a National Patient Safety Goal requiring that all behavioral health patients presenting to psychiatric and general hospitals receive suicide risk screening. However, upon examining data collected in ensuring years, it was discovered that over a quarter of hospital suicides occur on non-behavioral health units, and at-risk patients were passing through emergency departments, inpatient medical units, and outpatient clinics undetected.
In 2007, The Joint Commission (TJC) released a National Patient Safety Goal requiring that all behavioral health patients presenting to psychiatric and general hospitals receive suicide risk screening. However, upon examining data collected in ensuring years, it was discovered that over a quarter of hospital suicides occur on non-behavioral health units, and at-risk patients were passing through emergency departments, inpatient medical units, and outpatient clinics undetected.
This realization led TJC, in 2016, to recommend that all patients presenting to medical settings receive suicide risk screening. This recommendation led to the development of the Zero Suicide framework, which recommends universal patient screening for suicide risk at first contact and all subsequent contacts using the same tool and procedures.
How can universal suicide risk screening in primary care settings save lives?
Suicide is a global public health crisis and the 10th leading cause of death in the U.S. Research from TJC shows that at-risk individuals presenting at non-behavior health units may fall through the cracks and not receive the help they need.
Reasons for suicide risk screening in primary care settings:
- Many patients see PCPs instead of mental health professionals because of stigma, confidentiality concerns, and mental health provider shortages
- More than half of patients who have died by or attempted suicide visited a healthcare provider within a month of their death/attempt
- There is growing evidence to suggest screening program efficacy, particularly when paired with brief intervention and referral to treatment
Barriers and strategies for implementing suicide risk screening
 While there is little debate about why screening is important, questions arise about implementing screenings in primary care settings. In a 2020 case study, rural PCPs were interviewed about:
While there is little debate about why screening is important, questions arise about implementing screenings in primary care settings. In a 2020 case study, rural PCPs were interviewed about:
- Opinions toward universal suicide risk screening in rural primary care settings
- Barriers to suicide risk screening specific to their practices
- Interventions that would make universal suicide risk screening more feasible
Based on the interview findings, existing barriers and possible strategies for implementation were identified:
Barriers to implementation:
- Lack of access to mental health/crisis resources
- Disruption in clinic workflow
- Inadequate ability to follow-up with patients who screened positive for suicide risk
- Cultural beliefs, including fear of losing access to firearms
- General burdensomeness of screening in primary care
- Concerns about patient follow-up
- PCP discomfort with topic and lack of training in screening
Strategies for implementation:
- Use of technology or electronic medical records for screening
- Using a multidisciplinary team approach to screening
- Having standardized protocols for screening and assessment
- Having access to co-located behavioral health
- Additional training on the topic of suicide and suicide risk assessment
Considerations for implementing universal suicide risk screening in NW PA
 In addition to the barriers articulated by rural PCPs, there are social, cultural, and healthcare considerations for implementing universal screening:
In addition to the barriers articulated by rural PCPs, there are social, cultural, and healthcare considerations for implementing universal screening:
- Suicide rates are disproportionately higher in rural settings
- Stigma related to mental illness, confidentiality concerns, and mental health provider shortages are intensified in rural settings
- Rural settings more often have a lack of qualified medical and behavioral health providers, significant public transportation issues, more social isolation, increased access to lethal means, and region-specific environmental and cultural factors
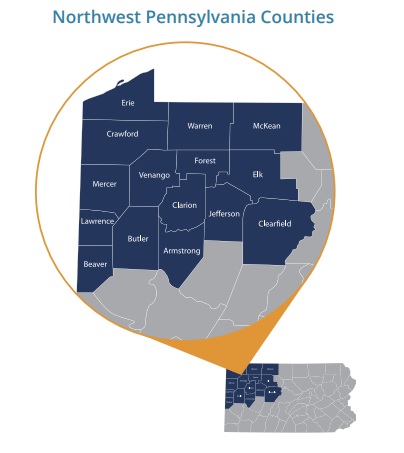
Because of these unique challenges, the NW PA Veteran Suicide Prevention Program is partnering with the 15 counties of NW PA to reduce Veteran suicide deaths. Health and behavioral health practices partnering with PERU will be trained and offered technical assistance in using the Zero Suicide framework to screen, treat, and refer patients to treatment and other services. Partners will also receive support to establish and enhance policies and procedures promoting mental and behavioral services among Veterans.
To learn more, visit the program website at theresilientveteran.org.
Need Help? Know Someone Who Does? Contact the National Suicide Prevention Lifeline at 1-800-273-TALK (1-800-273-8255) or use the online Lifeline Crisis Chat. Both are free and confidential. You’ll be connected to a skilled, trained counselor in your area.

